WCC Nursing Mission Statement
The mission of the nursing programs of the Alabama Community College System is to prepare graduates to practice safe, competent, patient-centered care in an increasingly complex and rapidly changing health care system. We seek to provide full and equal access to opportunities for education success to meet the community needs.
Nursing Philosophy
We believe that nursing is a dynamic profession, blending science with the use of evidence-based practice and clinical reasoning and the art of caring and compassion to provide quality, patient-centered care.
We believe learning is an interactive process in which faculty and students share responsibility to meet program outcomes. We believe in using educational methods that are current and supportive of students in the teaching and learning environment, with the presentation of information from simple to complex.
Nursing is guided by standards of practice and standards of professional performance. Standards reflect the values and priorities of the nursing profession. Therefore, we have integrated competencies from the National League of Nursing (NLN) into our philosophy as part of our core values.
Conceptual Framework
The conceptual framework derived, from the philosophy, forms a basis for the organization and structure of the nursing curriculum. This framework serves as a guide for nursing instruction in the attainment of student learning outcomes.
The framework consists of concepts that encompass the qualities of a successful graduate nurse. NLN competencies were chosen because they specifically define the competencies of the graduate Associate Degree Nurse and to achieve the goal of providing graduate nurses with the tools needed to provide holistic care in an every-changing health care delivery system. Each competency includes knowledge, skills, and attitudes to serve as a basis for consistent performance expectations across academic and practice settings.
Competencies
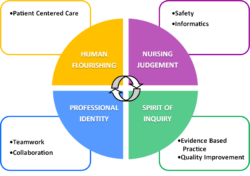
NLN competencies for nursing are central to the conceptual framework. The related QSEN competencies for graduate nurses define the knowledge, skills, and attitudes that the graduate nurse should possess to continuously improve the quality and safety of the healthcare systems within which they work. (QSEN)
- Human Flourishing: Advocate for patients and families in ways that promote their self-determination, integrity, and ongoing growth as human beings. (NLN, 2022)
- Patient-Centered Care: Recognize the patient or designee as the source of control and full partner in providing compassionate and coordinated care based on respect for the patient’s preferences, values, and needs. (QSEN, 2020)
- Nursing Judgment: Make judgments in practice, supported by evidence, that integrate nursing science in the provision of safe, quality care and promote the health of patients within the family and community context. (NLN, 2022)
- Safety: Minimize the risk of harm to patients and providers through both system effectiveness and individual performance. (QSEN, 2020)
- Informatics: Use information and technology to communicate, manage knowledge, mitigate error, and support decision-making. (QSEN, 2020)
- Professional Identity: Implement one’s role as a nurse in ways that reflect integrity, responsibility, ethical practice, and an evolving professional identity committed to evidence-based practice, caring, advocacy, and safe, quality care for diverse patients within a family and community context. (NLN, 2022)
- Teamwork and Collaboration: Function effectively within nursing and interprofessional teams, fostering open communication, mutual respect, and shared decision-making to achieve quality patient care. (QSEN, 2020)
- Spirit of Inquiry: Examine the evidence underlying clinical nursing practice to challenge the status quo, question assumptions, and offer new insights to improve the quality of care for patients, families, and communities. (NLN, 2022)
- Evidence-Based Practice: Integrate the best current evidence with clinical expertise and patient and family preferences and values to deliver optimal health care. (QSEN, 2020)
- Quality Improvement: Use data to monitor outcomes of care processes and apply improvement methods to design and test changes that continuously improve the quality and safety of health care systems. (QSEN, 2020)